- Announcing the AMA’s new precision education grant recipients
- Transforming Lifelong Learning Through Precision Education portfolio and grant program
- Precision Education Framework
- Supplement on precision education
- Watch on demand: Precision education
- Watch on demand: The next era of assessment
- Precision education: How it's advancing med ed
- Precision education plenary session at ChangeMedEd
- Producing a workforce that addresses the needs of the U.S.
- Reconnect medical education to patient care
- TRACERs Project
Announcing the AMA’s new precision education grant recipients
The American Medical Association recently announced the recipients of our new four-year, $12 million Transforming Lifelong Learning Through Precision Education grant program. An initial call for letters of intent in March 2025 yielded 197 ideas, from which the AMA requested 30 full proposals. After a rigorous review by the AMA’s Precision Education National Advisory Board, 11 teams were identified to receive grants and join our ChangeMedEd® Consortium.
Building on more than a decade of AMA leadership through our ChangeMedEd initiative, this investment underscores the AMA’s ongoing commitment to advancing medical education through innovation and collaboration.
See below for the list of the new AMA Transforming Precision Education Through Lifelong Learning grant recipients.
- Individualized Learning Plans for Precision Education
Grantee institution: A collaboration of 12 family medicine residencies led by Georgia Academy of Family Physicians (GAFP)
- Compassion in Motion: Training Tailored Communication Across the Clinical Continuum
Grantee institution: Louisiana State University Health Sciences Center
- Opening the Doors with the Right Education for the Right Student at the Right Time: The Continuum of Precision Education in Maryland's Newest Medical School
Grantee institution: Meritus School of Osteopathic Medicine (MSOM)
- Engaging Patients Toward Better Health: Using AI-based Ambient Listening to Improve Communication Skills of Trainees and Faculty in an Underserved Community-Based Setting
Grantee institution: Mount Sinai Morningside/West
- AI-Driven, Context-Aware, Precision Assessment of Individual and Team-Based Clinical Reasoning
Grantee institution: Perelman School of Medicine at the University of Pennsylvania
- Implementation and Evaluation of a Scalable, Sensor-Enabled Precision Learning Curriculum for Procedural Skills Certification Across the Continuum
Grantee institution: Stanford University
- Ambient AI for Precision Feedback: Augmenting Clinical Reasoning and Communication using Real-Time Feedback
Grantee institution: University of Cincinnati College of Medicine in collaboration with the Arizona State University John Shufeldt School of Medicine and Medical Engineering
- Developing Culturally Responsive AI for Rural Health: Utilizing Precision Education and Precision Coaching to Strengthen Hawaii’s Rural Physician Workforce
Grantee institution: University of Hawaii - John A. Burns School of Medicine
- Enhancing Precision Education Using “Feed-Back” and “Feed-Forward” Learning Analytics Data Systems: A Multisite Consortium Project to Align UME-GME Transitions
Grantee institution: A collaboration of 15 institutions, led by University of Illinois College of Medicine
- PACE: Precision Analytics for Coaching Effectiveness
Grantee institution: A collaboration of 36 anesthesia residency programs led by the University of Michigan
- Graduate Performance Profiles to Enhance Learning Analytics and Precision Program Improvement in Vascular Surgery
Grantee institution: A collaboration of seven vascular surgery residencies led by the University of Wisconsin School of Medicine and Public Health
Learn more about the grant recipients and program.
AMA announces new Transforming Lifelong Learning Through Precision Education portfolio and grant program
The AMA has announced its next endeavor to improve the health of the nation through medical education. Part of the AMA ChangeMedEd® initiative, the new AMA Transforming Lifelong Learning Through Precision Education portfolio will cultivate and promote democratization of the precision education ecosystem to offer individualized learning that aligns physician education with the needs of patients both now and in the future. By addressing the unique needs of each learner, precision education improves medical education from medical school through practice by boosting personalization, increasing efficiency and transferring agency to the learner.
The launch of this new portfolio culminates a two-year effort by the AMA to support the development of precision education, which leverages data and technology to increase personalization, efficiency and agency for learners.
The portfolio consists of two activities:
- Precision education grant program: The AMA will fund the development and implementation of precision education systems. Ten projects will receive funding of at least $1.1 million distributed over four years—with a total AMA investment of $12 million. Single U.S.-based institutions or groups of collaborating institutions that collectively have responsibility for the training of physicians at any stage of the continuum and sufficient influence over the context of training to implement proposed interventions are invited to apply for a grant. These institutions will join the ChangeMedEd® Consortium and work together to share findings, challenges and strategies, conduct collective evaluation and co-produce supporting tools for the responsible development and deployment of precision education systems. Access up-to-date information on the precision education grant program.
- Principles and standards development process: In collaboration with Medbiquitous, the standards development program of AAMC, AMA will convene experts to develop and promote adoption of data sharing principles and standards in precision education systems.
Learn more about the AMA’s work in precision education.
Check out the new AI resource in medical education.
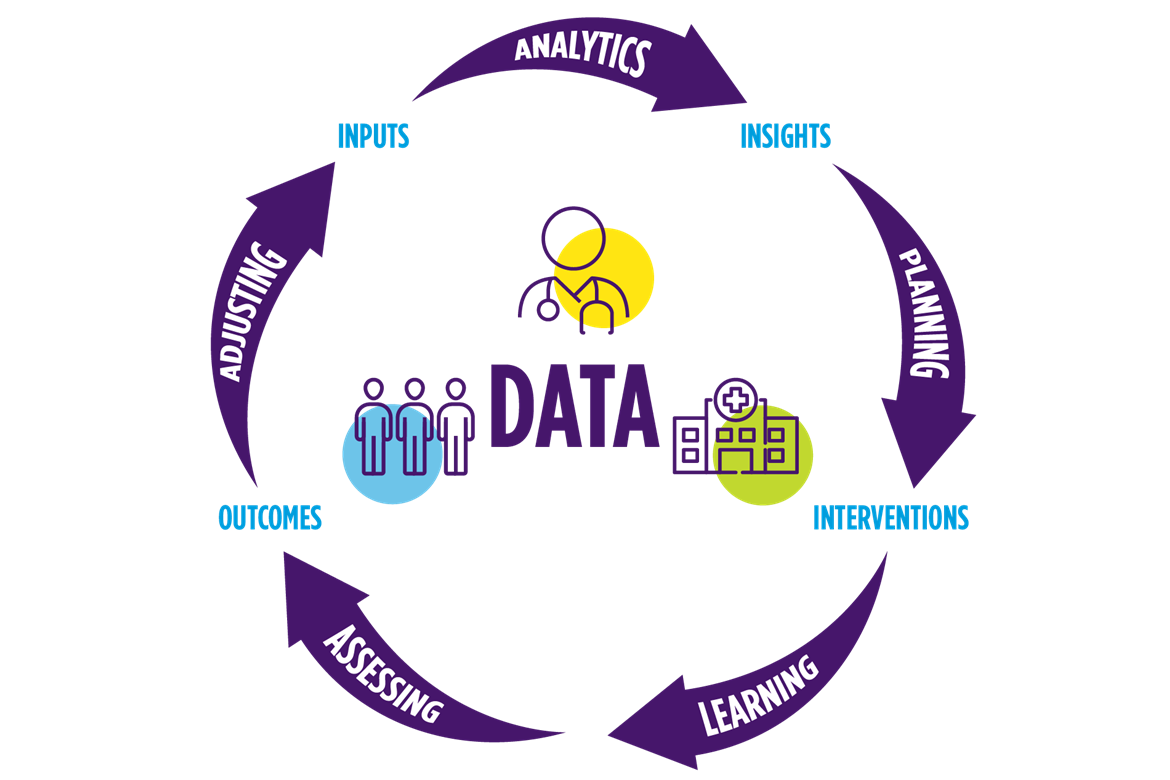
Precision Education Framework
The Precision Education Framework is the conceptual framework for an education system focused on individualized learning that aligns with learner needs as well as the needs of current and future patients. Data at the learner, program, or organization level anchors this cyclical system. Analytics applied to inputs generate insights. These insights drive planning processes and precision interventions. Assessed outcomes identify needs and determine adjustments. The cycle repeats as necessary.
The framework was initially proposed in: Desai et.al. Precision Education: The Future of Lifelong Learning in Medicine. Acad Med. 2024 Apr 1;99(4S Suppl 1):S14-S20
AMA Academic Medicine supplement on precision education
As part of the AMA ChangeMedEd initiative’s new strategic focus on precision education, the AMA supported a supplement in the April 2024 issue of Academic Medicine entitled, “The Next Era of Assessment: Advancing Precision Education for Learners to Ensure High-Quality, Equitable Care for Patients.”
In the supplement, authors compel readers to consider a next era of assessment that places less focus on how assessment is done (e.g., tests, work-based assessment) and more focus on why it is done: to ensure high-quality, equitable care for patients.
Watch on demand: Precision Education in Medical Education: On-the-Ground Initiatives and Learnings
This webinar features authors, Brian T. Garibaldi, MD, MEHP, and Eric Warm, MD, from the ChangeMedEd supplement in Academic Medicine who are taking novel approaches to apply precision education and use data and technology for effective assessment of learners at their own institutions. Watch now.
Watch on demand: The Next Era of Assessment: Equitable Patient Care and Precision Education for Learners
This webinar features guest editors from the AMA ChangeMedEd supplement in Academic Medicine and explore how the future of assessment–and the meaningful use of learning and data analytics in medical education–can focus on ensuring high quality equitable care. Watch now.
Dive deeper:
- How assessment can evolve to ensure high-quality, equitable care
- Bonus content: Listen to the Association of American Medical College recent Academic Medicine podcast on the next era of assessment and precision education, available on Apple, Spotify and wherever you listen to podcasts.
Precision education: What it is and how it's advancing med ed
Earlier this year, AMA published an article on an AMA issue brief on precision education and the future of lifelong learning in medicine.
Precision education plenary session at ChangeMedEd 2023
Presented during the September 2023 conference, this plenary reviews barriers to lifelong learning in medical education and how precision education can be an effective tool to improve the system.
Medical School Admissions: Focusing on Producing a Physician Workforce that Addresses the Needs of the United States
In this invited commentary, the authors acknowledge that the current system for selecting and developing the physician workforce is severely limited by the data available at all levels. Screening processes have relied on measures of convenience that are not well aligned with the desired attributes of physicians or of educational institutions. Innovations in data science and generative artificial intelligence platforms offer an opportunity for all stakeholders to act upon more meaningful information.
Reconnect medical education to patient care
Continuing professional development can be a source of frustration for practicing physicians with limited time. Often, structured training is not directly relevant to the physician’s practice and physicians rely heavily on just-in-time resources that may not support deeper learning.
A multi-disciplinary team at the AMA has developed Reconnect, an AI tool aiming to personalize physician lifelong learning and improve efficiency. Reconnect integrates with EHR systems (in a manner that does not transmit protected health information) to curate and deliver personalized education content relevant to a physician’s patient panel.
The algorithm identifies multivariate nuances within patient records and trends within a physician’s practice pattern to elevate appropriate learning resources in anticipation of upcoming clinic sessions. High-yield ongoing learning is the focus; this tool does not involve recommendations regarding the care of individual patients. The concept and prototype were developed over three years and is being piloted with health systems to test feasibility. Future study and refinement will pursue long term goals of enhancing physician well-being and improving care of patients.
The TRainee Attributable & Automated Care Evaluations in Real-Time (TRACERs) Project
This project builds on the concept of resident-sensitive quality measures (RSQMs). These are clinical care measures that are both important for patient care and highly attributable to an individual resident (rather than the team, system or patient). This project introduces the concept of TRainee Attributable & Automated Care Evaluations in Real-Time (TRACERs), which are characterized as: meaningful for patient care and trainees; sufficiently attributable to the trainee of interest; automatable, meaning there is minimal human input needed once fully implemented; scalable across electronic health records (EHRs) and training environments; and amendable in real-time to formative educational feedback loops.
TRACERs builds upon RSQM research by automating the previously labor-intensive process of EHR data extraction and exploring how to make such measures scalable across institutions. This undertaking is a collaboration between researchers from the University of Cincinnati College of Medicine, NYU Grossman School of Medicine and Stanford University School of Medicine.