As physicians, we hear firsthand from the media and other places how health care costs are out of control, and we’re often asked what can be done to control those costs. A new analysis from the AMA helps shed some light on how the health care dollar is spent, and reveals that costs aren’t as out of control as we may think.
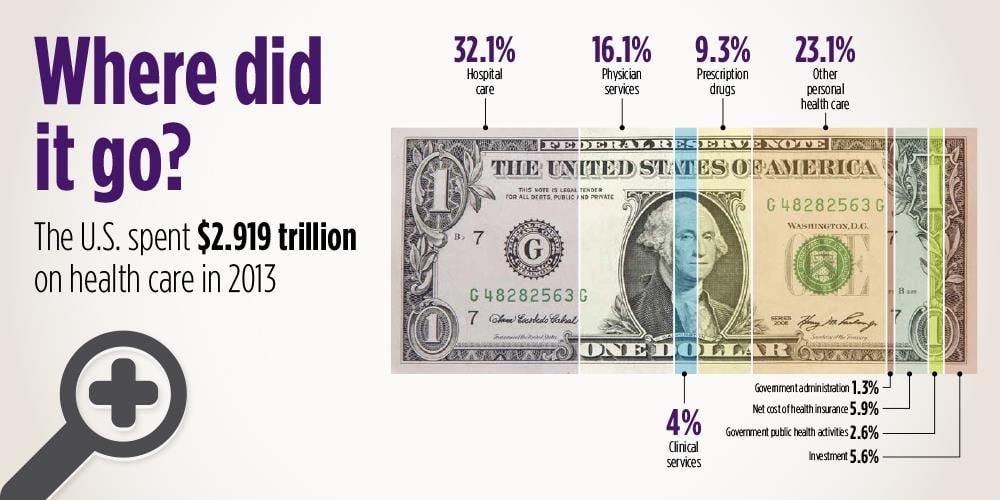
This analysis shows how health care is financed and where the money goes. In 2013, the last year for which data are available, national health expenditures were more than $2.9 trillion—that breaks down to $9,255 per person. This reflects growth of only 3.6 percent over the previous year—the lowest annual growth rate since 1961, the first year the current framework for spending was used.
And that data doesn’t stand alone. The past five years have been characterized by slow growth in spending.
What’s interesting is that out of that $2.9 trillion, only 16.1 percent went to physician services. Moreover, physicians are part of the reason that spending is at historically low growth levels. Physician spending grew more slowly over the 2003-2013 period than hospital spending, clinical spending and total personal health spending.
The largest piece of this spending pie goes to hospital care—about 32 percent. But acute care often is preventable. That’s why my clinic seeks to keep our patients out of the hospital. Through an aggressive approach to managing cancer treatments and its side effects, we keep our patients as healthy as possible, minimizing emergency room visits and hospitalizations. By offering same day appointments many practices in multiple specialties can intervene in a patient’s problem and avoid admissions.
Lowering costs through innovation
At my clinic, we manage the overall care for our patients, handle insurance issues, take care of scheduling and more. All the patient has to do is show up.
We found that offering same-day appointments and encouraging patients to call us before racing to the emergency room—along with some other changes—reduced overall health care costs. This new delivery model kept patients out of the hospital and became a way to deliver cost-effective care.
I was awarded a grant from the Center for Medicare and Medicaid Innovation (CMMI) three years ago to take what we’d done at this first clinic, the New Mexico Cancer Center, and replicate it in six other practices across the country.
We’ve started what we call Community Oncology Medical Homes (COME HOME) to test how oncology private practices can provide better care for patients with cancer at lower costs. Now we have worked with the American College of Surgeons to obtain Commission on Cancer accreditation. By keeping patients out of the hospital and handling what we can in physician offices, we expect to realize significant cost savings. You can read more about my work in this area in another Viewpoints post.
Here’s another way we can minimize health care costs: Addressing the burdens of chronic diseases.
The AMA is doing this now by working to prevent cardiovascular disease and type 2 diabetes—and improving outcomes for people with these conditions.
For example, we recently launched a new multi-year partnership with the Centers for Disease Control and Prevention: Prevent Diabetes STAT: Screen, Test, Act—Today™. The partnership will help physicians connect patients to diabetes prevention programs in their communities or online. We also have released a guide to help physicians set up self-measured blood pressure monitoring programs in their practices, which can empower patients to get high blood pressure under control.
And we also can lower our own costs by reducing what we spend on administrative burdens and increasing our efficiency in our practices. Last week, I wrote a post about the ways the AMA is making that possible.
Tell us: How are you reducing costs in your practice? Let me know in the comments below.