- Opportunity to enhance timely access to care
- Use of technology to accelerate BHI adoption and impact
- Defining practical solutions for stakeholders
- Value framework in action
- Making accessible, equitable treatment a reality
- Webinar recording: BHI and digitally enabled care
- Additional AMA resources
- 988 Suicide & Crisis Lifeline
Opportunity to enhance timely access to care
The AMA, in collaboration with Manatt Health, developed a report articulating the opportunities and challenges of incorporating virtual care (telehealth) and other digital tools to accelerate the adoption of behavioral health integration (BHI).
A diverse working group representative of physician practices, large employers, health plans and patient advocates was convened to contribute to and inform the generation of this report.
The goal of this work is threefold:
- Define the opportunities and limitations to incorporating technology to advance BHI.
- Define practical solutions that stakeholders can pursue to advance digitally enabled BHI.
- Demonstrate how to use AMA's Return on Health framework to measure the value of digitally enabled BHI models.
This effort builds on the AMA's ongoing efforts to advance BHI adoption by physician practices, alongside our Return on Health framework, which defines the various ways in which virtual care programs are generating, and can generate, value.
Use of technology to accelerate BHI adoption and impact
Combating the growing mental health crisis
The U.S. is in the midst of a decades-long mental health crisis that has been exacerbated by the COVID-19 pandemic. BHI is essential to reaching more individuals who need mental health treatment and solving the nation’s growing mental health crisis. Stakeholders across the health care system have committed to addressing this crisis; however, the long-standing shortage of mental health providers, among other persistent challenges, has limited timely access to treatment.
Shift to hybrid care models (in-person and telehealth)
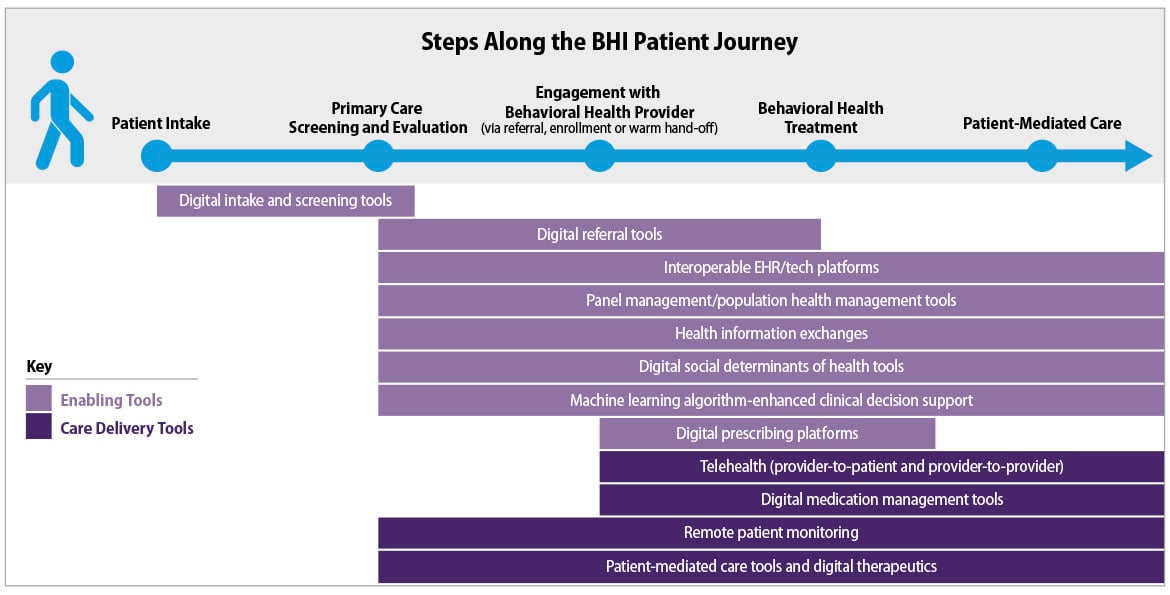
The current shift within the U.S. health care system toward hybrid models that fully integrate in-person and virtual care presents a unique opportunity to enhance the overall effectiveness of BHI. Technology can enhance patient management and treatment, support integration, limit fragmentation of care and ultimately generate value for both patients and providers throughout the BHI patient journey within primary care.
Defining practical solutions for stakeholders
The report includes comprehensive, practical solutions that stakeholders—physician practices and systems, health plans and coverage programs, federal and state policymakers, employers and private or publicly-traded behavioral health companies—can pursue to advance digitally enabled BHI. For example:
- Physician practices and health systems: Increase behavioral health diagnosis and treatment rates by incorporating evidence-based digital health solutions and enabling technology into standard workflows.
- Health plans: Increase BHI adoption by expanding coverage and fair payment with a margin for all stakeholders utilizing the Collaborative Care Model (CoCM) and other BHI models.
- Policymakers (Federal): Grow the behavioral health workforce by increasing federal funding for efforts such as loan forgiveness and new residency and training programs.
- Employers: Reduce out-of-pocket costs for employees seeking care by evaluating how and when to apply cost-sharing.
- Private or publicly-traded behavioral health companies: Generate robust clinical and economic evidence for digitally enabled BHI by working with stakeholders to develop national standards for BHI technologies.
Value framework in action
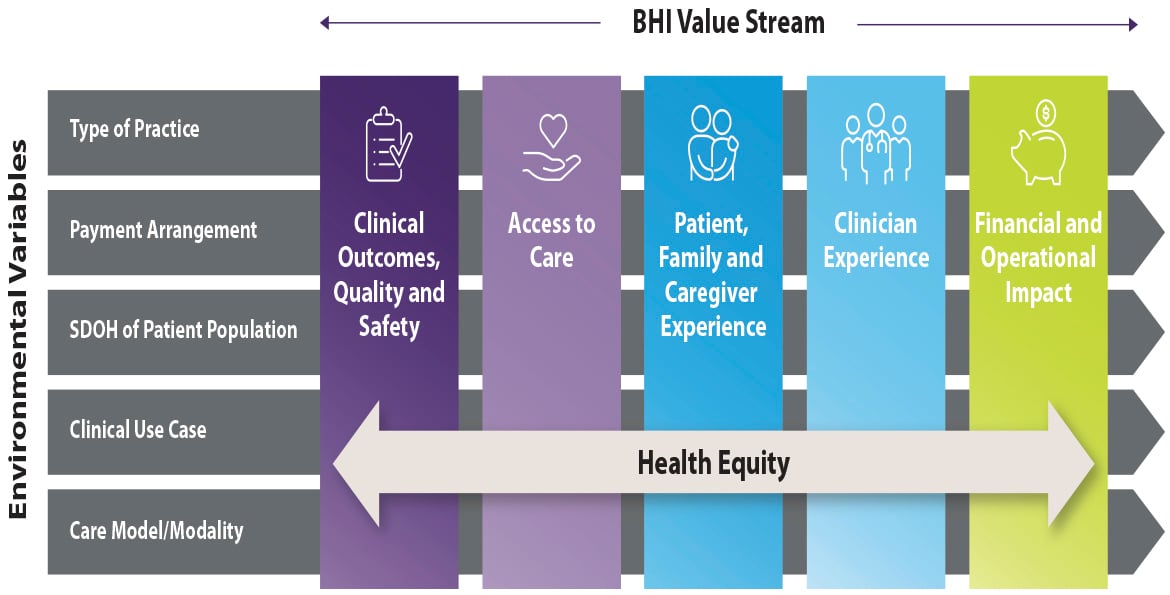
Demonstration of the comprehensive value that BHI generates for providers, patients and society at large could further drive adoption among primary care specialists. The value framework presented in the AMA's Return on Health report is a useful tool that can be used to achieve this aim.
Making accessible, equitable treatment a reality
There is ample evidence that BHI produces superior patient outcomes, improves patient experience and access to care, and can generate cost savings. All stakeholders have a critical role to play in making accessible and equitable treatment that addresses peoples’ mental and physical health needs a more standard practice within primary care.
Thanks to our generous contributors for sharing their experiences and expertise in the development of the report Accelerating and Enhancing Behavioral Health Integration Through Digitally Enabled Care: Opportunities and Challenges (PDF).
Webinar recording: BHI and digitally enabled care
This webinar from the AMA and Manatt Health examines the opportunities and challenges of accelerating BHI through digitally enabled care, with examples from innovators and researchers applying practical solutions for supporting the widespread adoption of sustainable BHI.
Additional AMA resources
- Behavioral health integration in physician practices
- AMA's Return on Health: Telehealth framework for practices
- AMA strategic behavioral health guides for patient care
988 Suicide & Crisis Lifeline
With an increased number of people reporting worsening mental health in recent years, it is imperative that people are aware of the 988 Suicide & Crisis Lifeline (formerly known as the National Suicide Prevention Lifeline) telephone program.
People experiencing a suicidal, substance use, and/or mental health crisis, or any other kind of emotional distress can call, chat or text 988, and speak to trained crisis counselors. The national hotline is available 24 hours a day, 7 days a week.
The previous National Suicide Prevention Lifeline phone number (1-800-273-8255) will continue to be operational and route calls to 988 indefinitely.