If you’re preparing for the United States Medical Licensing Examination® (USMLE®) Step 1 exam, you might want to know which questions are most often missed by test-prep takers. Check out this example from Kaplan Medical, and read an expert explanation of the answer. Also check out all posts in this series.
This month’s stumper
A 45-year-old man comes to the physician because of increased frequency of urination. He voids approximately 12 times a day and three times each night. He describes the inability to maintain an erection but reports no decrease in libido. Physical examination shows that he is oriented to person and place, but not to time.
He is 5 feet, 10 inches tall and weighs 240 pounds; BMI is 34 kg/m2. He has an elevated waist-to-hip-ratio. Cardiac auscultation reveals an audible S1 and S2, with a regular rate and rhythm. The lungs are clear.
There are no palpable abdominal or scrotal masses. Urinalysis shows 3+ glucose and is negative for ketones. Fasting serum glucose is 195 mg/dL and the fasting insulin level of 78 mIU/L (normal: less than 25mIU/L).
Which of the following blood laboratory findings in serum is most likely in this patient?
A. Decreased concentration of C-peptide.
B. Elevated anion gap.
C. Elevated concentration of β-hydroxybutyrate.
D. Increased antibodies against islet cell proteins.
E. Increased osmolality.
The correct answer is E.
Kaplan Medical explains why
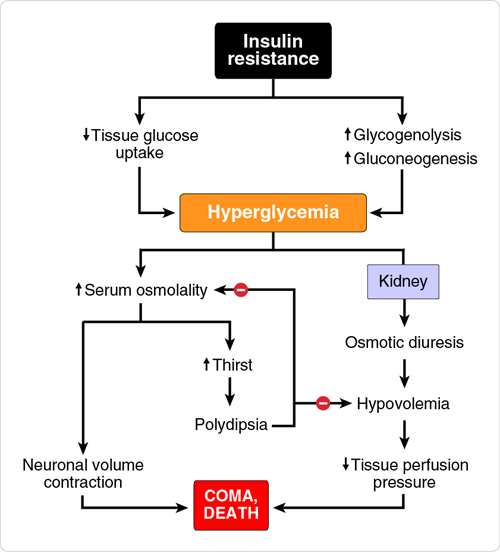
This patient likely has early stage type 2 diabetes mellitus based on his increased fasting insulin and glucose levels, increased urinary frequency, nocturia, erectile dysfunction and obesity. The condition is characterized by insulin resistance resulting in hyperglycemia and increased serum osmolality.
The dehydration associated with osmotic diuresis makes the hyperosmolality worse. As the osmolality increases above 330 mOsm/kg H2O, the loss of water from neurons to extracellular fluid is sufficient to produce coma. In non-ketotic, hyperosmolar coma, blood glucose values can range from 800–2,400 mg/dL and produce serum osmolalities of 330–440 mOsm/kg H2O.
Why the other answers are wrong
Choice A: Pancreatic β cells secrete insulin and C-peptide in a 1:1 ratio. Since the patient's fasting insulin levels are increased, serum C-peptide levels would be increased (not decreased) also. In the early stage of type 2 diabetes, insulin resistance produces a compensatory pancreatic β-cell hyperplasia and increased insulin levels. As the disease progresses, β cell function declines and insulin levels fall.
Choice B: Anion gap typically widens in patients with type 1 diabetes due to accumulation of ketone bodies. Even small amounts of insulin are sufficient to prevent ketosis, however, so patients with type 2 diabetes typically do not develop an elevated anion gap or ketoacidosis.
Choice C: β-hydroxybutyrate (also known as 3-hydroxybutyrate) is a ketone body that can accumulate in patients with type 1 diabetes with very low insulin levels. Our patient has type 2 diabetes with serum insulin levels sufficiently high to suppress ketogenesis and a rise in β-hydroxybutyrate concentrations.
Choice D: Type 2 diabetes is not associated with increased circulating antibodies. There is a significant autoimmune component to type 1 diabetes, with autoantibodies targeting insulin, glutamic acid decarboxylase and insulinoma-associated protein, among other islet cell antigens.
Tips to remember
- A patient who is obese and has glucosuria, but not ketonuria, likely has type 2 diabetes mellitus.
- Type 2 diabetes is characterized by insulin resistance, which leads to hyperglycemia and increased serum osmolality.
For more prep questions on USMLE Steps 1, 2 and 3, view other posts in this series.
The AMA and Kaplan have teamed up to support you in reaching your goal of passing the USMLE® or COMLEX-USA®. If you're looking for additional resources, Kaplan provides free access to tools for pre-clinical studies, including Kaplan’s Lecture Notes series, Integrated Vignettes, Shelf Prep and more.