If you’re preparing for the United States Medical Licensing Examination® (USMLE®) Step 1 exam, you might want to know which questions are most often missed by test-prep takers. Check out this example from Kaplan Medical, and read an expert explanation of the answer. Also check out all posts in this series.
A 23-year-old man with a history of resistant asthma is brought to the emergency department because of an acute onset of shortness of breath and dyspnea. He had treated himself with medication at home prior to calling for help. While in the emergency department, he develops palpitations, agitation and a tremor in both his hands.
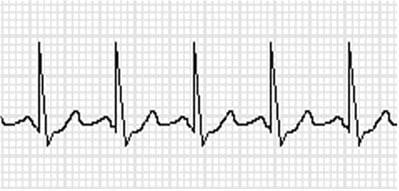
His temperature is 37.2 °C (98.9 °F), pulse is 120 beats a minute, respirations are 22 breaths per minute, blood pressure is 132/87 mm Hg, and oxygen saturation is 95% on room air. An ECG is shown. Before acute asthma treatment is started, the patient suddenly develops seizures.
The drug most likely responsible for this patient's symptoms acts by which of the following mechanisms?
A. β2-receptor agonism.
B. Competitive blockade of muscarinic receptors.
C. Inactivation of NF-κB transcription factor.
D. Inhibition of phosphodiesterase and adenosine receptors.
E. Mast cell stabilization.
Subscribe and succeed in medical school
Get tips and insider advice from the AMA on succeeding in medical school—delivered to your inbox.
The correct answer is D.
Kaplan Medical explains why
In this question, the patient comes to the emergency department because of an acute asthma attack. While in the emergency department, he becomes agitated, develops a tremor, and later has a seizure. Furthermore, the patient's vital signs and ECG readings (every P-wave is followed by a normal-looking QRS) suggest that he has sinus tachycardia, with the heart rate above 100 beats a minute. These symptoms are occurring as a result of a medication that he took prior to coming to the emergency department. Based on this information and his current symptomatology, the patient likely has early signs of theophylline toxicity.
While some β-agonists such as salmeterol have been associated with increased tremor and arrhythmia, they rarely lead to neurotoxic events such as seizures. Theophylline has a very narrow therapeutic index, and careful measures must often be taken to control the patient's plasma levels of the drug. Theophylline is a methylxanthine generally used as a late second line or third line agent for the treatment of asthma due to its unfavorable side effect profile.
Though the mechanism of action of theophylline remains unclear, most evidence suggests that it inhibits phosphodiesterase and antagonizes adenosine receptors.
Why the other answers are wrong
Choice A: Albuterol is a β2-receptor agonist that is often administered as a rescue medication in the emergency department. Unlike the longer lasting salmeterol, it is less commonly associated with tremors and tachyarrhythmia when administered by inhalation. This agent is associated with central nervous system stimulation, transient increases in blood pressure and mild tachycardia.