Helping patients obtain accurate SMBP results
Blood pressure (BP) constantly fluctuates in most people. Taking multiple BP measurements each day, for multiple days in an environment where a person spends a significant amount of time, yields a more accurate and representative picture of that person's true BP. When compared with a single, conventional office BP measurement, SMBP measurements taken over a week are much more predictive of future cardiovascular risk. Training patients to properly prepare for and perform SMBP is essential to obtaining accurate measurements.
Ensuring use of validated blood pressure measurement devices
Blood pressure measurement devices used by patients for out-of-office measurements should be validated for clinical accuracy. Validated devices have passed an international validation protocol performed by independent skilled BP measurement experts. A preliminary list of BP measurement devices sold in the United States that meet criteria for the US Blood Pressure Validated Device Listing™ was made available on April 29, 2020. Additional validated BP measurement devices sold in the U.S. may be found on international validated device listings that are maintained by Canadian, European and British and Irish organizations.
Patients should use automated BP measurement devices with upper arm cuffs of appropriate size. Many devices are sold with cuffs that will fit arm circumferences within the small adult to large adult range, but not all devices have extra-large cuff sizes available. Using an inappropriately sized cuff can lead to inaccurate BP measurements, as can using cuffs on different areas of the body (e.g., finger cuffs). A wrist cuff should only be used if an upper arm cuff is not clinically appropriate or if an appropriately sized upper arm cuff is not available.1
Because it is recommended that patients take SMBP measurements for 7 days, devices with the capacity to store at least 7 days of measurements (28 or more readings) are preferred.1
Selecting a SMBP cuff size
Blood pressure (BP) measurement devices with upper arm cuffs provide the most accurate measurements.1 Wrist cuffs are not recommended for clinical use unless patients cannot use upper arm cuffs due to arm size or other medical reasons.1 Finger devices are also not recommended for clinical use because these are less accurate than upper arm BP measurement devices.1
Below are steps to determine the appropriate upper arm cuff size. If possible, it may be easier for patients to have another person assist with the process.
Ask patients to gather the following items:
- Tape measure
- BP measurement device, cuff and manual (if device is already purchased)
Locate mid-upper arm:
- Measure the length of the arm between the acromion process (bony protuberance on shoulder) and the olecranon process (bony protuberance at elbow)
- Divide the distance in half to locate the mid-upper arm
Determine arm circumference:
- Wrap a tape measure around the mid-upper arm to determine arm circumference (typically measured in centimeters)
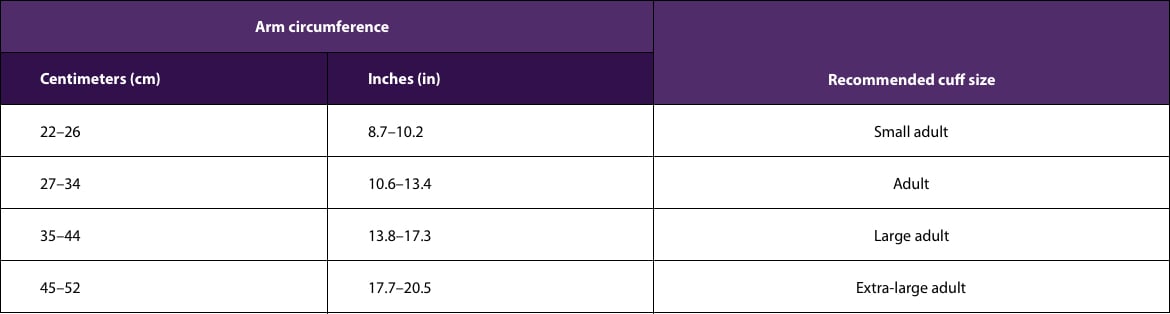
Determine cuff size:
- Based on arm circumference, determine the cuff size that is appropriate. Use this information to help with device selection. Many BP measurement devices have circumference ranges printed directly on the cuffs. This information can also often be found in the device manual or on the device box.
Modified from Table 3 in: Muntner P, Shimbo D, Carey RM, Charleston JB, et al. Measurement of blood pressure in humans: a scientific statement from the American Heart Association. Hypertension. 2019;73:e35–e66. doi: 10.1161/HYP.000000000000008.
Access the 7-step SMBP quick guide
The guide highlights seven key steps physicians and care teams can take to use SMBP with patients 18 years and older with high blood pressure, and includes links to useful supporting resources.
Essential AMA resources
- SMBP training video
- SMBP training video (Spanish)
- SMBP infographic (available in 18 languages)
- SMBP recording log
- SMBP CPT® coding
- SMBP Coverage Insights: Medicaid
- SMBP Policy Brief: Medicaid (PDF)
- SMBP benefits for patients with Medicaid
References
1 Muntner P. Shimbo D. Carey RM. et al. Measurement of blood pressure in humans: A scientific statement from the American Heart Association. Hypertension. 2019;73(5):e35-e66. doi: 10.1161/HYP.0000000000000087.
Disclaimer: These steps are for informational purposes only. These steps are not intended as a substitute for the medical advice of a physician; they offer no diagnoses or prescription. Furthermore, this information should not be interpreted as setting a standard of care or be deemed inclusive of all proper methods of care, nor exclusive of other methods of care reasonably directed to obtaining the same results. This protocol reflects the best available evidence at the time that it was prepared. The results of future studies may require revisions to the recommendations in this protocol to reflect new evidence, and it is the clinician's responsibility to be aware of such changes.