If you’re preparing for the United States Medical Licensing Examination® (USMLE®) Step 1 exam, you might want to know which questions are most often missed by test-prep takers. Check out this example from Kaplan Medical, and read an expert explanation of the answer. Also check out all posts in this series.
This month’s stumper
A 68-year-old woman is brought to the emergency department because of shortness of breath and a 4.5 kg (10 lbs.) weight gain over the past two weeks. Her pulse is 105 per minute and blood pressure is 160/84 mm Hg. Physical examination of the neck reveals bilateral jugular venous distension. The abdomen is soft and nontender but a positive fluid wave is present. The extremities show 2+ bilateral pitting edema. She is admitted to the medicine service for treatment. Intravenous furosemide is administered and diuresis of 5 L of fluid occurs in a relatively short time. The following data were collected from the patient before and after receiving furosemide.
Which of the following is the most likely explanation for the acid-base abnormality in this patient?
A. Decreased plasma aldosterone.
B. Hyperkalemia.
C. Hyperventilation.
D. Hypoventilation.
E. Loss of extracellular fluid.
The correct answer is E.
Kaplan Medical explains why
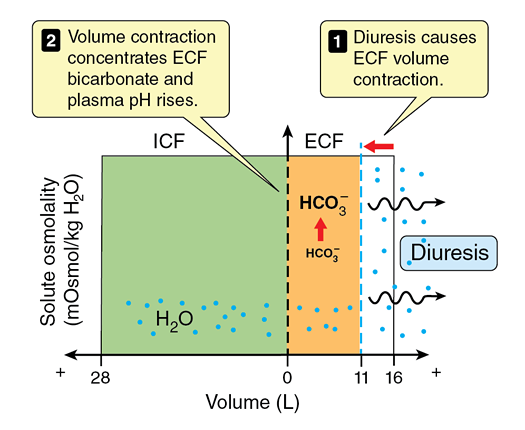
The patient is showing the signs and symptoms of "contraction alkalosis," a type of metabolic alkalosis caused by diuretic-induced loss of extracellular fluid.
Loop diuretics (such as furosemide) and thiazides can cause rapid and significant urinary fluid excretion, as seen in our patient. This decreases extracellular fluid (ECF) volume and hence relieves symptoms associated with edema, but it concentrates ECF HCO3-, causing a metabolic alkalosis. In our patient's case, furosemide treatment has decreased ECF volume by 5L, causing [HCO3-] to rise from 24 mEq/L to 35 mEq/L, and serum pH to rise to 7.49.
Activation of the renin-angiotensin-aldosterone system (RAAS) following ECF volume contraction further potentiates the alkalosis:
- darr ECF volume rarr darr Arterial pressure rarr RAAS activation.
- Angiotensin II stimulates Na+-H+ exchange in the proximal tubulerarr uarr H+ secretion.
- Aldosterone stimulates the apical V-type H+-ATPase in the distal segments rarr uarr H+ secretion.
Why the other answers are wrong
Choice A: Decreased plasma aldosterone levels would tend to cause acidosis, not alkalosis. Diuretics decrease ECF volume and activate RAAS (as discussed above). Aldosterone levels would be expected to be increased in our patient following rapid diuresis of 5L of fluid.
Choice B: Hyperkalemia is often associated with a metabolic acidosis rather than a metabolic alkalosis. Various mechanisms and pathways are involved.
Choice C: PCO2 is increased in our patient, which would be more consistent with hypoventilation, not hyperventilation. Hyperventilating increases the rate of CO2 transfer to the atmosphere, so arterial PCO2 falls.
Choice D: Hypoventilation does increase arterial PCO2, as seen in our patient, but CO2 retention results in a respiratory acidosis, not a metabolic alkalosis. The patient is retaining CO2 in attempts to compensate for the acid-base disturbance.
Tips to remember
- Contraction alkalosis is a type of metabolic alkalosis caused by loop diuretics.
- Loop diuretics cause salt and water to be excreted, whereas bicarbonate is retained.
- Loss of ECF volume increases plasma bicarbonate concentration.
For more prep questions on USMLE Steps 1, 2 and 3, view other posts in this series.
The AMA and Kaplan have teamed up to support you in reaching your goal of passing the USMLE® or COMLEX-USA®. If you're looking for additional resources, Kaplan provides free access to tools for pre-clinical studies, including Kaplan’s Lecture Notes series, Integrated Vignettes, Shelf Prep and more.