If you’re preparing for the United States Medical Licensing Examination® (USMLE®) Step 2 exam, you might want to know which questions are most often missed by test-prep takers. Check out this example from Kaplan Medical, and read an expert explanation of the answer. Also check out all posts in this series.
This month’s stumper
A 62-year-old truck driver arrives at the emergency department with significant shortness of breath. He denies any significant medical problems. He has smoked two packs of cigarettes per day for the last 40 years. His family history is significant for hypertension and coronary artery disease. His vital signs are temperature 38.4 ºC (101.1 ºF), blood pressure 128/64 mm Hg, pulse 112 per minute, respirations 24 per minute, and oxygen saturation 87 percent on room air. The physical examination is significant for decreased breath sounds, with crackles at the bases bilaterally. Arterial blood gas analysis reveals:
pH – 7.4
PCO2 – 32 mm Hg
PO2 – 54 mm Hg
HCO3 – 20 mEq/l
CBC shows
Hb – 14.8 g/dL
Hct – 43%
WBC – 4,500/mm3
Neutrophils – 94%
Lymphocytes – 2%
Monocytes – 2%
Eosinophils – 1%
Basophils – 1%
Platelets – 256,000/mm3
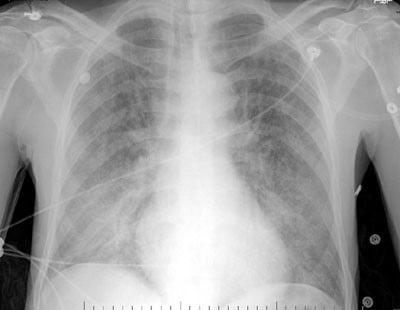
Chest x-ray is shown below.
What is the most definitive diagnostic study that should be obtained?
A. Basic metabolic panel.
B. Bronchoscopy with bronchoalveolar lavage.
C. CT scan of the chest.
D. Immunofluorescence of induced sputum sample.
E. Liver function tests.
The correct answer is D.
Kaplan Medical explains why
This patient presents with shortness of breath and fever. Physical examination is significant for bilateral crackles, and the arterial blood gas shows hypoxia. The chest x-ray film indicates bilateral lower lung field infiltrates. These nonspecific findings are suggestive of severe pneumonia.
Why the other answers are wrong
Read these explanations to understand the important rationale for why each answer is incorrect.
Choices A and E: Neither a basic metabolic panel nor liver function tests would aid in the diagnosis of P. jiroveci pneumonia.
Choice B: The low lymphocyte count (2 percent of 4,500 = 90 lymphocytes/mm3, thus CD4 must be even lower), however, is suggestive of immunocompromised status. HIV and Pneumocystis jiroveci (formerly carinii) pneumonia (PJP/PCP) are very likely possibilities in this patient. Immunofluorescence of an induced sputum sample is required for the definitive diagnosis of PJP.
If the test is negative in a patient for whom there is high clinical suspicion of PJP, bronchoscopy with bronchoalveolar lavage is warranted. The frequency of PJP infection has decreased with increased awareness of HIV, but it still may be the presenting sign of AIDS.
Choice C: A CT scan of the chest may be necessary with advanced disease, as it is helpful in determining the extent of the disease. It will suggest the diagnosis of PCP pneumonia, but it is not the definitive diagnostic study.
Tips to remember
- Suspect PCP pneumonia in an immunocompromised patient presenting with shortness of breath, fever, and radiologic evidence of bilateral interstitial pneumonia.
- The diagnosis is established on immunofluorescence of an induced sputum sample.
The AMA and Kaplan have teamed up to support you in reaching your goal of passing the USMLE® or COMLEX-USA®. If you're looking for additional resources, Kaplan provides free access to tools for pre-clinical studies, including Kaplan’s Lecture Notes series, Integrated Vignettes, Shelf Prep and more.
For more prep questions on USMLE Steps 1, 2 and 3, view other posts in this series.