The economic impact of COVID-19 on health care continues to reveal itself through reductions in patient volume and revenue and in higher practice costs. As the pandemic stretches on, physician practice viability remains under threat.
Physician financial impact research findings
Financial impacts were assessed with a claims-based analysis of changes in Medicare physician spending for 2020 and a nationwide survey of physicians in July and August of 2020.
Medicare physician spending
This updated report (PDF) provides an in-depth look at impacts of the COVID-19 pandemic on physicians. Using Medicare claims data, the report documents changes in Medicare Physician Fee Schedule (MPFS) spending for 2020, highlighting the types of service, settings and specialties that were most affected by the pandemic.
Key findings from the report
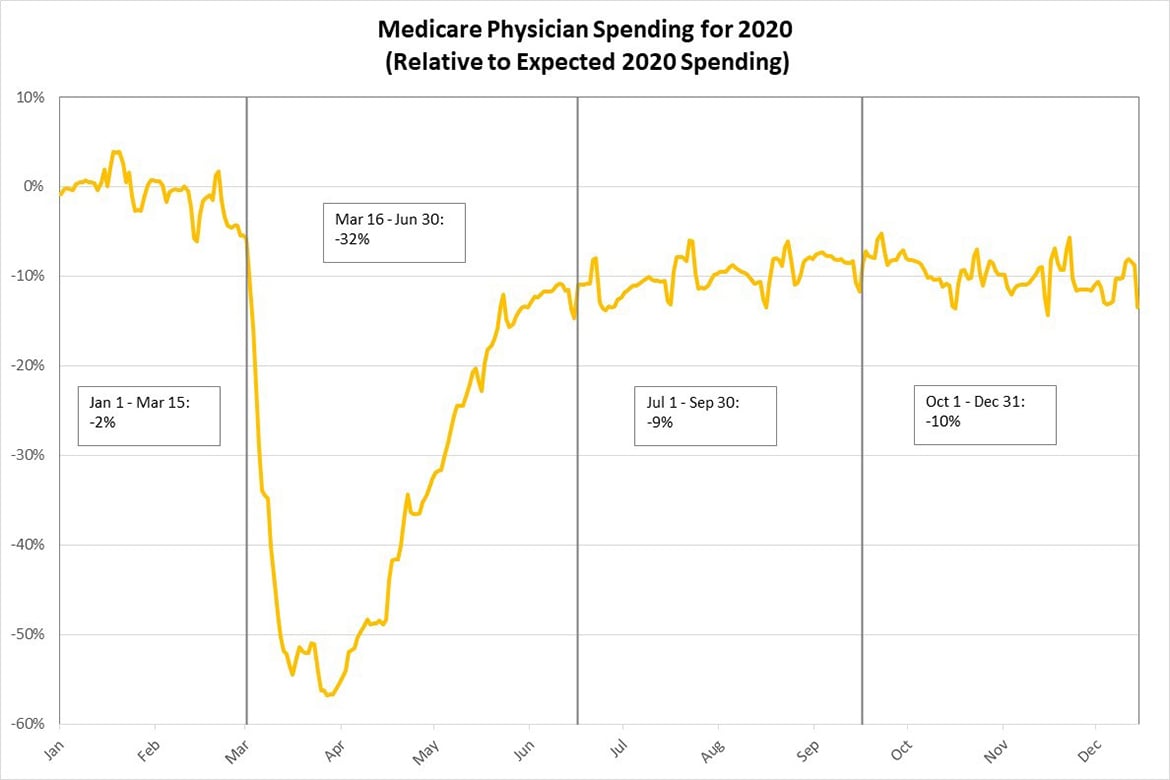
- MPFS spending dropped sharply in March and April of 2020, falling as much as 57% below expected.
- Although it recovered from the April low, MPFS spending in the fourth quarter of 2020 was still 10% less than expected.
- For all of 2020, the estimated reduction in Medicare physician spending associated with the pandemic was $13.9 billion (a 14% decrease compared to expected).
- An estimated 39% of Medicare fee-for-service enrollees received a telehealth service in 2020, up from less than 1% in 2019.
Related correspondence
- March 2, 2021: Sign-on letter to U.S. Senate
- March 5, 2021: Letter to U.S. House of Representatives
- February 12, 2021: Letter to U.S. House of Representative
Additional key findings
- By specialty, physical therapists (-28%) saw the biggest reduction in spending and physician specialties that were particularly hard-hit included otolaryngology (-24%), cardiac surgery (-20%) and ophthalmology (-19%).
- At the state level, impacts ranged from a 9% reduction in Oklahoma to a 22% reduction in Minnesota.
- Telehealth accounted for 5% of MPFS spending in 2020 (up from less than 0.1% prior to the pandemic) but use was concentrated in a handful of service categories.
COVID-19 financial impact survey results
The AMA commissioned a nationwide survey of patient care physicians in July and August of 2020 to assess the financial impacts of the COVID-19 pandemic. The results, based on the responses of 3,500 physicians, illustrate the precarious trends and realities facing physician practices.
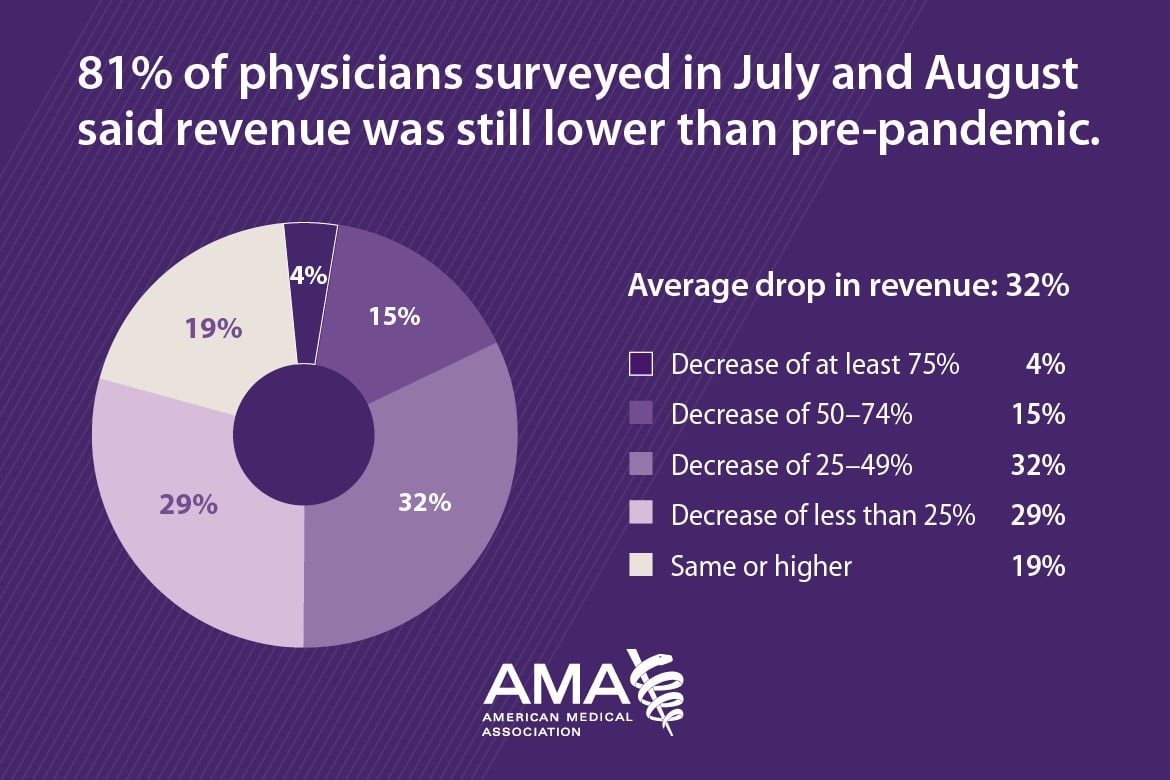
- 81% of physicians surveyed in July and August of 2020 said revenue was still lower than pre-pandemic.
- Average drop in revenue: 32%
Telehealth coverage
Even with eased telehealth coverage restrictions, telehealth services did not offset reduced in-person patient visits.
- 81% of physicians were still providing fewer in-person visits when surveyed in July and August of 2020 than pre-pandemic.
- Average in-person visits fell from 95 to 57 per week.
- At the height of use, weekly telehealth visits were almost 5 times higher than pre-pandemic.
- At the time of the survey, weekly telehealth visits were still almost 3 times higher than pre-pandemic levels.
- Almost 70% of physicians, despite telehealth increases, were still providing fewer total visits (in-person + telehealth) at the time of the survey than pre-pandemic.
- Average total visits fell from 101 to 72 per week.
Use of Personal Protective Equipment (PPE)
A significant expense: New safety practices require use of more PPE. Supplies were difficult to acquire—especially for smaller practices that lack purchasing power or vendor relationships to compete with larger health systems in the marketplace.
- 64% of practice owners said that spending on PPE was up from pre-pandemic. Average increase in PPE spending was 57%.
- 36% of physicians said that acquiring PPE was very or extremely difficult. Difficulties were more acute for smaller practices and those that were physician-owned.
Federal financial relief
Federal financial relief early in the pandemic was helpful and appreciated but the core revenue issues these programs were intended to address remain. The vast majority of practice owners said federal financial assistance programs were very or extremely helpful.
- CARES Act
- Medicare Accelerated and Advanced Payment Program
- SBA Paycheck Protection Program
Negative impact of COVID-19 on physician practices
It is clear the COVID-19 pandemic continues to have a negative impact on physician practices both in terms of decreased revenue and increased costs. While initial federal financial relief programs were helpful to practices that applied, it appears the road to recovery, particularly for smaller physician-owned practices, remains difficult and more economic relief is needed.