Nearly 700 physicians and medical students are gathering this week just a few miles away from Capitol Hill for the 2023 AMA Interim Meeting, where they will consider proposals across a wide range of clinical practice, payment, medical education and public health topics.
But there is one issue that is clearly at the top of agenda for the AMA House of Delegates: The need to stop the 3.37% Medicare physician pay cut set for 2024 and enact broader Medicare reforms to ensure that the 65 million Americans who rely on it have continued access to high-quality physician care.
That 2024 pay cut “is an unfortunate continuation of a two-decade march in making Medicare unsustainable for patients and physicians,” AMA President Jesse M. Ehrenfeld, MD, MPH, said last week, noting that it would come atop this year 2% pay cut and at the same time that the Medicare Economic Index (MEI) has risen 4.6%. That’s the highest MEI this century, and comes after 2023’s 3.8% increase.
The combination is “a recipe for financial instability,” said Dr. Ehrenfeld, an anesthesiologist in Wisconsin. “Patients and physicians will wonder why such thin gruel is being served.”
Learn how you can take part in the fight to reform Medicare on behalf of your patients and practices at the AMA's Fix Medicare Now website. Join physicians nationwide in telling Congress to cancel the cut.
It’s been bad. It’s getting worse.
In his statement, Dr. Ehrenfeld noted that “physicians routinely have faced cuts in the last two decades. Yet,” he added, “there is nothing routine about the past few years.”
Doctors have worked to save lives and continue to meet patients’ chronic care needs throughout the COVID-19 pandemic, and have persevered through the ensuring burnout. They also have seen the costs of running a medical practice soar even as Medicare payment updates have offered little to no relief.
“There is widespread acknowledgement that access to care is being threatened,” Dr. Ehrenfeld said. “The declining revenues in the face of steep cost increases disproportionately affect small, independent, and rural physician practices, as well as those treating low-income or other historically minoritized or marginalized patient communities.”
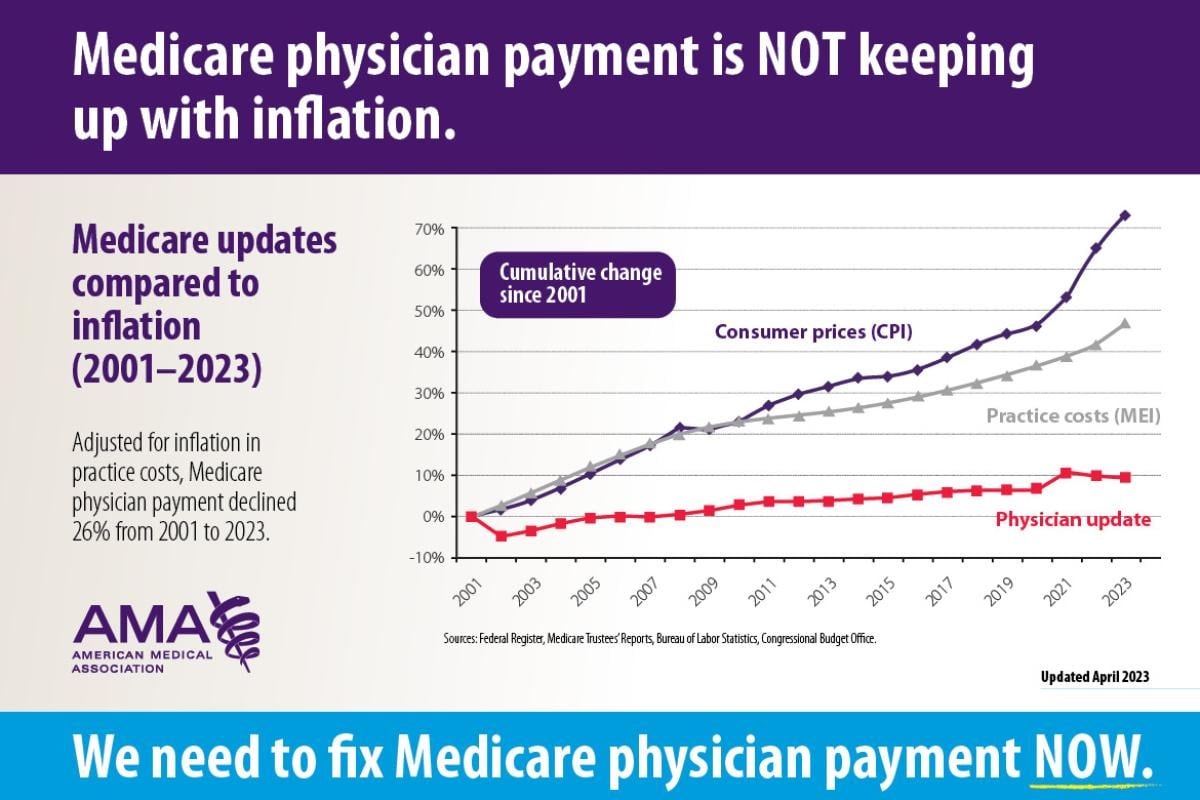
After adjusting for inflation, Medicare physician payment has effectively declined 26% from 2001 to 2023—and that is before the 2024 pay cuts are factored in.
Nonpartisan experts are recognizing the unsustainability of the Medicare physician payment system. This spring, for the first time, the Medicare Payment Advisory Commission recommended a physician payment update tied to the MEI. And in their March report, the Medicare Trustees said they “expect access to Medicare-participating physicians to become a significant issue in the long term” unless Congress takes steps to bolster the payment system.
Leading the charge to reform Medicare pay is the first pillar of the AMA Recovery Plan for America’s Physicians.
The AMA has challenged Congress to work on systemic reforms and make Medicare work better for you and your patients. Our work will continue, fighting tirelessly against future cuts—and against all barriers to patient care.
Bipartisan fixes are at hand
Already, the AMA and other physician organizations have backed practical solutions to fix Medicare now. They include H.R. 2474, the Strengthening Medicare for Patients and Providers Act, which has been co-sponsored by a bipartisan group of more than 50 members of Congress. The bill would give physicians an annual, permanent inflationary payment update in Medicare tied to the MEI.
Physician organizations also called for key parts of discussion drafts of the Provider Reimbursement Stability Act to be enacted. Among other things, the proposal would raise the budget-neutrality threshold from $20 million to $53 million and increase every five years by the cumulative rise in MEI since the last update to the threshold. Importantly, it would also provide a mechanism for CMS to revise budget-neutrality adjustments in the event that original utilization estimates were too high, so that money is not inappropriately and permanently removed from the physician payment pool.
“Medicare reform is moving to the top of many agendas, no doubt spurred by seniors and people with disabilities concerned by the prospect of disappearing access,” Dr. Ehrenfeld noted last week after the CMS final Medicare physician pay schedule was issued.
And it assuredly remains true this week at the AMA Interim Meeting in National Harbor, Maryland, just across the Potomac River from Capitol Hill. Dr. Ehrenfeld will address delegates at the opening session Friday night, with the need to fix Medicare now expected to be a central theme of his remarks.
The House of Delegates works in a democratic process to create a national physician consensus on emerging issues in public health, science, ethics, business and government to improve the care and public health of patients and communities. The policies adopted at this meeting will give the AMA direction and act as a driving force on the future of American medicine.
At the 2023 AMA Annual Meeting in June, delegates declared Medicare physician payment reform to be an urgent advocacy and legislative priority.
To help physician advocates and lawmakers get a stronger grasp on the complicated terrain of Medicare physician payment reform, the AMA's Medicare Basics series provides an in-depth, straightforward look at key elements of the payment system and why they are in need of reform—including budget-neutrality rules.