Creating greater customization for collecting patient information in electronic health records (EHR) may improve documentation timeliness and reduce stress for residents and attending physicians, according to a new study. Find out how one resident clinic improved its documentation process and dramatically increased physician satisfaction.
Switching from free-text to structured data forms
While EHRs can offer observed patient benefits, “there is evidence that the use of EMRs cause work disruption, which may delay documentation of patient encounters,” the study, which was published in Academic Medicine, said. This compelled researchers and professors at Vanderbilt School of Medicine to host an EHR-based intervention that would “improve compliance with institutional standards of documentation of well child checks for residents and attending physicians without increasing stress,” according to the study.
The intervention was hosted at the Children’s Hospital Primary Care Clinic at Vanderbilt, which is staffed by 74 residents and supervised by 17 attending physicians. The institutional standards at Vanderbilt University require residents to complete their documentation within three days and attendings to complete their attestations within 14 days. The process for doing so used free-text notes in StarPanel, a Web-based EHR specifically built for Vanderbilt.
For the study, researchers created an alternate approach that streamlined the process using a collection process more specific to the patient. They created 18 age-specific, structured data entry forms for residents and attendings to use for point-of-care documentation instead of free-text notes.
The new forms included age-appropriate risk screening questions and anticipatory guidance recommendations from the American Academy of Pediatrics Bright Futures Guidelines. They also featured “specific areas for parental concerns and interval history, nutrition and sleep elimination information, developmental screening questions … and embedded links to growth curves, including body mass index,” according to study authors.
More timely documentation, less resident stress
All residents and attendings at the clinic participated in the intervention. Researchers monitored their documentation completion rates and derived patient data for an average of 231 patient visits per month. Using pre- and post-intervention surveys, they also assessed participants’ stress and satisfaction levels related to documentation.
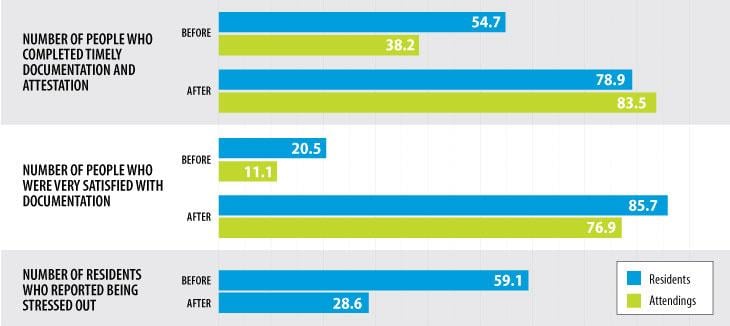
The alternate documentation approach increased the median percentage of resident documentation and physician attestations completed within Vanderbilt’s required timeframe from:
- 54.7 percent to 78.9 percent for residents
- 38.2 percent to 83.5 percent for attendings
After the intervention, the number of people who reported high satisfaction with documentation increased dramatically, from:
- 20.5 percent to 85.7 percent for residents
- 11.1 percent to 76.9 percent for attendings
As a result, residents reporting stress with documentation was cut in half, from 59.1 percent to 28.6 percent.
Although authors acknowledge the limitations of this study, the intervention’s marked success suggests that it may be a beneficial approach to explore further. The authors now are teaching computer-based documentation in exam rooms.
Improving EHRs to support physicians, patient care
The shortcomings of EHRs that present roadblocks to high-quality patient care are a source of constant concern for many physicians. As part of its Professional Satisfaction and Practice Sustainability initiative, the AMA is working with physicians, vendors, policymakers, health care systems and researchers to drive EHR improvements that can advance care delivery.
Learn more about the 8 top challenges and solutions identified by practicing physicians and health IT experts.