In his last year of medical school, Maurice G. Sholas, MD, PhD, worked in a spinal cord injury unit. He immediately found his passion and became a pediatric physical rehabilitation physician in New Orleans. And, as fate would have it, Dr. Sholas became the first pediatric physical rehabilitation physician in the state of Louisiana. Drawn to complex problems, Dr. Sholas takes great pride in being among the hundreds of physicians who subspecialize in this type of care and continues to fight for his patients with disabilities.
“As a pediatric rehabilitation doctor, what I do clinically is take care of acquired or congenital physical disabilities,” said Dr. Sholas, also a member of the AMA Ambassador Program, which equips individuals with the skills and knowledge to confidently speak to the AMA's initiatives and the value of AMA membership.
“I look at the whole kid in the context of their family, their community, their hopes and their dreams,” he said. “To do that, I use specialty equipment and medications, and I can use interventions from my physical, occupational and speech pathologists, but the point is to manage the consequences of the disability so the kid can be as functionable as possible.”
In an interview, Dr. Sholas discussed being a pediatric physical rehabilitation physician and how he advocates for patients with disabilities and those from historically marginalized racial and ethnic groups.
AMA: How has the COVID-19 pandemic affected children with disabilities?
Dr. Sholas: What's really hard is that kids with disabilities are too often isolated. They tend to not have as large and dynamic a peer group. They tend to go to doctor appointments and to their school or school-like activities, but there's not—depending on your community—as many vocational opportunities for you as typically developing kids. So, when you take a kid like that, and the whole world shuts down and they were already isolated, it kept them in a bubble.
The good consequence of that is that bubble protected them from infection. However, that bubble was pierced by what their parents had to do to make it. If you think about it, for Black families, only one in four could do remote work at the peak of COVID. Latinx families, only one in five could do remote work. So, Black and brown families were much more likely to have to choose between protecting their family and providing a living.
You're seeing that Black and brown children in these households were, one, more likely to be exposed than other kids whose parents could do remote work to a greater degree. And two, there was this massive shift from people who had jobs—especially jobs in hospitality industries—to public insurance. And we know that when you're on Medicaid, you have a harder time finding therapists and you have a harder time finding specialists.
The last piece to really think about in all of this is a lot of hospitals went to emergency-only services and diverted all nonessential care and elective care, which means peds departments in general were shut down. It was very hard for my patients to schedule appointments with me when the hospitals were on diversion as all of their resources were going to dealing with the massive influx of COVID-19 patients.
When you have kids in lower socioeconomic statuses who depend on the emergency room for care because they don’t necessarily have the greatest relationship with a primary care doctor or don’t have a primary care doctor, that’s even more difficult.
AMA: How do you continue to help your patients with disabilities during the pandemic?
Dr. Sholas: What's exciting to me is that as a Black man in medicine, I am one of 3% of physicians. I was the first Black man board certified in my field and it's absurd that we're in this still talking about the first of anything, but this is where we are.
So, part of my goal in orientation is that I believe in advocating with my platform, my agency, and my voice. That's how I'm oriented and how I have to be to make a way for places and spaces that weren't for me.
It's a natural thing for me to talk for kids with disabilities because they're the highest users of our health care system. They require some of the most care and they don't vote. This is who I am—I believe a good doctor requires you to be a good citizen first.
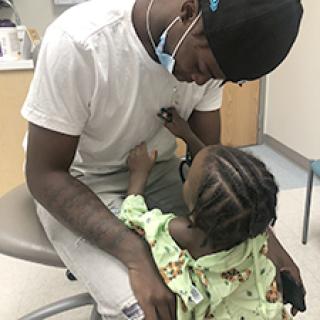
AMA: Is that what is represented in the photo you shared on Twitter of a young boy holding a stethoscope up to his brother’s chest?
Dr. Sholas: That little baby has spastic diplegic cerebral palsy, so he is just on the verge of walking and my interventions injecting botulinum toxin into his spastic muscles in his legs let him go from not being able to walk to being able to walk.
That boy would come to see me and he would say, “Doctor,” and he would take my stethoscope and do imitation play showing he knew what that stethoscope was for and what I did. Him listening to his brother's heart, that broke me. I had to go to the bathroom, cry a little bit because those are the things that come with doing my job.
Outside of me providing care for this kid, I put a spark in him that may or may not have come another way. To hear my Black patients specifically—their parents say, “My kid hates all doctors and can't wait to come see you,” that’s where it’s at. They have someone who looks like them, sees them and sees their family.
AMA: How does pediatric rehabilitation differ from rehab medicine delivered to adult patients?
Dr. Sholas: In children, you have the added twist of growth and development. When you rehabilitate adults it’s about, “I used to be able to walk. I need to learn to walk again.” If you come in as a child and you're 9 months old, you never walked. So technically it's not rehabilitation—you’re habilitating them.
You have to figure out what you are trying to get them to, based on not just their age, but their developmental abilities and goals. They may be 24 months by the calendar, but they’re just starting to stand and cruise and try to take independent steps. They’re 10 months functionally, so you can’t plan based on their being 24 months old. You plan based on what they’re able to do. And what they’re able to do shifts over time.
Another example is there’s no problem with a 2-month-old, a 10-month-old or a 2-year-old using a diaper—5-year-olds do not use diapers. That particular child who uses a diaper up until they go to kindergarten is not vastly different than their peers, but their inability to control their bowels and bladder doesn’t mean their disease got worse. It just means that as you develop and grow, we expect you to do more stuff and they may not get to that stuff. That’s a key difference.
AMA: What ways do you advocate for the historically marginalized racial and ethnic groups your patients with disabilities are part of?
Dr. Sholas: My big project right now is emPOWER NOLA. We are a Robert Wood Johnson Clinical Scholars group that focuses on creating trauma-informed spaces in the community. We do that by harnessing the power of our culture bearers and our naturally occurring social networks.
AMA: What can other physicians and health systems do to improve reach and care for patients with disabilities?
Dr. Sholas: Be mindful in how you plan things. For example, a big health system in Florida decided they wanted to do an inpatient peds rehab unit and create more peds rehab services, but they put their hospital in a location that was not accessible by public transportation. So how are poor or middle-income families going to get to these brand-new facilities?
Similarly, if you build a hospital that is accessible by multiple types of transportation, do you have valet parking? If you don’t, how exactly is someone supposed to bring their kid, their wheelchair and all their equipment to an appointment and park? Those are ways—small and large—that hospital systems and physicians can be intentional with making my kind of patients feel welcomed.
I tell all of my hospital administrators and my colleagues to think about them and intentionally provide for them. Have a flat high-low table that you can lower so they transfer on it and raise. So you can examine the patients, have lifts available in your exam rooms so your nurses don’t blow their backs out transferring all these patients. I’m simply saying: Think about things you can do to be intentional.
AMA: What else is important to know?
Dr. Sholas: I believe in organized medicine because small subspecialties like mine don't have the bandwidth or the numbers to really move big issues. But when you get me in a room with fellow physicians and people who are interested in kids with disabilities, you really harness the power of people and understanding care.
I'm a big advocate. I'm on the board of the National Medical Association. I'm a member of the American Medical Association, American Academy of Physical Medicine and Rehabilitation, and my state society. And I'm the current president of the New Orleans Medical Association because—despite all the work I do as an individual—we need to harness our collective talents, power and resources to move the whole ball forward.