Even though significant progress has been made in improving high blood pressure control rates in the U.S., almost half of adults have elevated BP. To perform proper blood-pressure measurement and maintain control in your patients—and to help improve their overall health—make sure your workflow includes these three important questions.
A wealth of tips for addressing blood pressure are available through Target: BP™, a joint initiative between the AMA and American Heart Association (AHA) to improve blood-pressure control and build a healthier nation.
In addition to direct access to trained field-support specialists, a data platform and a suite of evidence-based tools and resources offered by the AMA and the AHA, Target: BP offers annual, recurring recognition for all participating sites that achieve hypertension control rates of 70 percent or higher among their adult patient population year over year.
In 2018, nearly 800 organizations have been recognized for their efforts focusing on blood pressure control within the populations they serve.
“Were you rushing to get here or physically active right before this appointment?” There are multiple factors that can influence blood pressure measurement. To eliminate inaccurate readings, make sure to position your patient properly.
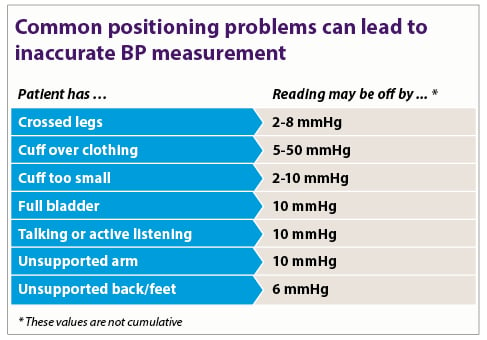
Common positioning problems can lead to inaccurate BP measurement, which can have a serious impact on the numbers you use to diagnose and determine treatment. Patients should have time to rest before you check their blood pressure and should be sitting quietly. Use the chart at the right as guidance to make sure the patient’s blood pressure isn’t falsely elevated.
“Have you been taking your medication?” If patients are on medication for high blood pressure, it is important to know if they are actually taking it. Costs, complicated regimens and side effects can all be reasons why patients stop using their medication.
Make sure you are discussing any factors that may prevent them from sticking to their treatment plan. Nonadherent patients will struggle to live well with chronic conditions. Bringing the right attitude to discussing the problem goes a long way in improving patients’ medication adherence.
“What’s your diet and physical activity regimen like?” If a patient chooses unhealthy foods or abstains from physical activity, find out why. Direct the patient to community resources that can help with proper diet and exercise.
Following through on lifestyle recommendations may be challenging for some patients with poor social support, obstacles to exercise and healthy foods, and challenging finances. When possible, partner with your patients who need support from local partners and connect with organizations that can help. And don’t forget to explain how eating healthy foods and staying active can help lower blood pressure.
An AMA membership means you’re motivating millions to control hypertension. When the nation’s health is on the line, you can count on the AMA to be part of the solution.