If you’re preparing for the United States Medical Licensing Examination® (USMLE®) Step 2 exam, you might want to know which questions are most often missed by test-prep takers. Check out this example from Kaplan Medical, and read an expert explanation of the answer. Also check out all posts in this series.
This month’s stumper
A 55-year-old woman with a history of oxygen-dependent COPD comes to the emergency department with worsening shortness of breath and chest pain. The chest pain is described as mostly right-sided and constant but worse with deep inspiration. The pain and shortness of breath awoke her from sleep in the middle of the night and she called emergency medical services to bring her to the emergency department.
Her temperature is 37 °C (98.6 °F), blood pressure 170/70 mm Hg, pulse 133 beats a minute, and respirations 28 per minute. Oxygen saturation is 83% on 6 L of oxygen by nasal cannula. She is in moderate respiratory distress and is using accessory muscles to breathe.
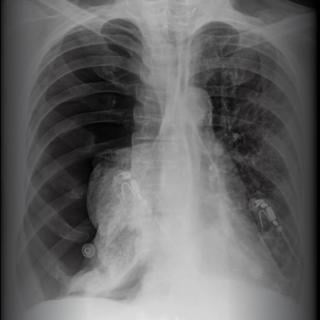
Her heart rate is tachycardic and regular. The lungs have decreased breath sounds on the right side more than on the left. There are scattered wheezes on the left. The remainder of her physical examination is normal. Stat chest x-ray is shown.
Which of the following is the most appropriate next step in management?
A. Albuterol, ipratropium bromide, oxygen, antibiotics, and steroids.
B. Aspirin, heparin, oxygen, metoprolol, and nitrates.
C. IV heparin.
D. Intercostal chest tube in the left lung.
E. Intercostal chest tube in the right lung.
The correct answer is E.
Kaplan Medical explains why
This patient has a right-sided pneumothorax secondary to emphysema. Although a pneumothorax (if small enough) can resolve spontaneously, many require chest-tube insertion. This patient has a large right-sided pneumothorax that can be recognized on chest x-ray film as the lack of peripheral lung markings on the right with radiographic hyperlucency.
Treatment of clinically significant pneumothorax is insertion of a chest tube with negative pressure to allow lung re-expansion. Remember, in the emergent setting of a tension pneumothorax, a needle may be inserted quickly to let out air.
Why the other answers are wrong
Choice A: Albuterol, ipratropium bromide, oxygen, antibiotics and steroids is the treatment for a COPD exacerbation. Although this patient has a history of COPD, it is more likely that her pneumothorax is causing her acute worsening symptoms, such as pleuritic chest pain, shortness of breath, and decreased breath sounds on the right side.
These findings, along with the chest x-ray, make pneumothorax the most likely diagnosis. Chest radiographs are almost always ordered in patients presenting with a COPD exacerbation to evaluate for a cause, such as pneumonia.
Choice B: Combination aspirin, heparin, oxygen, metoprolol and nitrates is the treatment for acute coronary syndrome. No evidence is presented to suggest that this patient has cardiac ischemia.
Choice C: IV heparin administration is the treatment for pulmonary embolism (PE). PE could explain the patient's shortness of breath and chest pain, but the chest x-ray film suggests an alternative diagnosis.
Choice D: The left side of the lung is normal, demonstrating lung markings emanating from the hilum to the periphery.
Tips to remember
- When facing sudden dyspnea in an emphysematous patient, always think of pneumothorax as a probable cause.
- Pneumothorax on chest radiograph is identified by lack of lung markings.
- Treatment is chest-tube placement.
For more prep questions on USMLE Steps 1, 2 and 3, view other posts in this series.
The AMA and Kaplan have teamed up to support you in reaching your goal of passing the USMLE® or COMLEX-USA®. If you're looking for additional resources, Kaplan provides free access to tools for pre-clinical studies, including Kaplan’s Lecture Notes series, Integrated Vignettes, Shelf Prep and more.