New physician-reported data are revealing how the Affordable Care Act (ACA) has affected doctors’ practices in terms of patient mix by insurance status. More of their patients are covered and fewer lack insurance, with the improvement on this critical score seen most in the states that expanded Medicaid under the ACA.
The one-of-a-kind survey looks beyond the already well-established decline in the number of uninsured—down to 27 million from 45 million prior to the ACA’s implementation—by reporting how the change has actually played out in physician experience at a wide range of medical practices. The analysis, taken from results of the AMA’s Physician Practice Benchmark Surveys, provides the most up-to-date breakdown of coverage type—Medicare, Medicaid, commercial plans, uninsured and a smattering of “other” payers—seen at physician practices. It also gives a comparative view of before and after the 2014 implementation of key ACA provisions.
“The results regarding changes in patient mix between 2012 and 2016 are consistent with changes in the insurance coverage of the population. As a percentage of their patients, physicians saw more Medicaid and privately insured patients in 2016 than they did in 2012, and the average uninsured patient share declined,” according to the survey report.
“However, the changes for Medicaid and uninsured patients were only statistically significant in states that chose to expand their Medicaid programs under the ACA.”
Nineteen states, mostly in the southeastern and central parts of the country, decided to forgo the ACA’s Medicaid expansion provisions. Nationally, Medicaid enrollment increased by more than 15 million from 2013 to 2016, compared with roughly 11 million people who enrolled through ACA exchanges.
“The most striking difference,” the report notes about expansion versus non-expansion states, “was in the percentage of physicians with uninsured patients. While this fell by more than 7 percentage points in expansion states, the drop in non-expansion states was only 2.2 percentage points.”
Physicians’ eye view
The report provides a recent snapshot of medical practices’ patient panels by type of insurance coverage and the proportion those patients represent in an average physician’s patient mix. The report says fresh information was needed because “nationally representative data on patient mix from the physician’s perspective is either fairly limited or dated.”
Overall, the report demonstrates that most physicians see a range of patients by coverage type, though there are some marked differences based on specialty.
In 2016, on average, nearly all respondents—98 percent—saw privately insured patients and most—89.3 percent—had Medicare patients. Medicaid and uninsured patients were also seen by most physicians—82.6 percent and 75.6 percent, respectively.
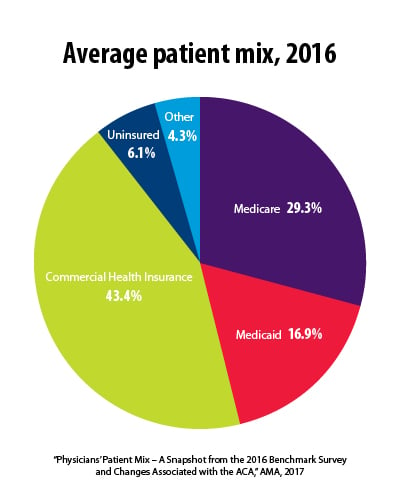
Patients with commercial health insurance make up the biggest single share of physicians’ patients—43.4 percent—but that still falls short of the percentage covered by public programs. Combined, government payers Medicare and Medicaid—at 29.3 percent and 16.9 percent—on average made up the biggest segment. Uninsured patients, on average, constituted 6.1 percent of patient mix. The category of “other”—which includes workers’ compensation claims—filled out the balance.
As expected, the average proportions varied markedly by specialty. Pediatricians and obstetrician-gynecologists reported the smallest Medicare population and the largest commercial health insurance share. The specialists seeing the highest share of patients covered by Medicaid were pediatricians and psychiatrists. Surgeons, internal medicine and its subspecialties, and radiology, all had substantial Medicare patient loads—each more than a third. The specialty with the largest uninsured patient load—an average of 14.2 percent—was, perhaps not surprisingly, emergency medicine. Emergency physicians had the lowest share of patients covered by commercial health insurance, 29.1 percent.
While the report underscores a significant increase in patients with Medicaid coverage in expansion states, it also found that workload is not being picked up evenly. “Although Medicaid enrollment increased sharply over this period due to the ACA, we did not see a significant increase in the percentage of physicians treating Medicaid patients,” the report notes. “Instead, the Benchmark Survey data suggest those that those participating in the program took on a larger Medicaid patient load in 2016 compared to participants in 2012.”
This and nearly all of the comparative data in the report were reflected in single-digit changes and not all were statistically significant at the 5 percent level, the standard used in nearly all cases. For example, although the percentage of physicians who saw Medicaid patients in non-expansion states went up from 80.9 percent to 82.5 percent, it did not represent a statistically significant rise.
The survey, conducted by the AMA’s Division of Economic and Health Policy Research, captured responses from post-residency physicians actively involved in patient care, from around the country and the full range of medical specialties, but not employed by the federal government.
The analysis was formally released as part of the AMA’s Policy Research Perspectives series, and is titled “Physicians’ Patient Mix—A Snapshot from the 2016 Benchmark Survey and Changes Associated with the ACA.” Benchmark surveys in the series have been conducted in 2012, 2014 and 2016, with about 3,500 respondents each year, and cover practice arrangements and payment methodologies, and include reports on changes in physician ownership of medical practices and physician participation in new payment models.